Selective serotonin reuptake inhibitor drugs (SSRIs) are among the most commonly prescribed medications for depression, anxiety disorders, obsessive‑compulsive disorder and several other psychiatric conditions. Because their name highlights serotonin, many people assume SSRIs simply replace serotonin or “fix” a serotonin deficiency, however the reality is more nuanced. Here we will take a look at how SSRIs work, what the evidence says about serotonin deficit, why symptoms often improve only after weeks of treatment with SSRIs and the side effects and risks you should know before starting—or stopping—an SSRI.
How SSRIs Work
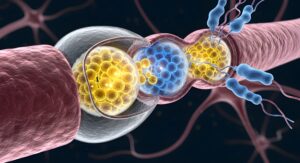 More than providing a simple serotonin boost, selective serotonin reuptake inhibitor drugs work by blocking the serotonin transporter protein (SERT) that normally reabsorbs serotonin in the brain, so that more serotonin stays available between nerve cells. By inhibiting SERT, SSRIs raise the concentration of serotonin in the synapses between the cells, increasing the chance serotonin will activate receptors on the receiving neuron. However, although the immediate increase of extracellular serotonin is measurable, people usually don’t feel better right away.
More than providing a simple serotonin boost, selective serotonin reuptake inhibitor drugs work by blocking the serotonin transporter protein (SERT) that normally reabsorbs serotonin in the brain, so that more serotonin stays available between nerve cells. By inhibiting SERT, SSRIs raise the concentration of serotonin in the synapses between the cells, increasing the chance serotonin will activate receptors on the receiving neuron. However, although the immediate increase of extracellular serotonin is measurable, people usually don’t feel better right away.
When using SSRIs, improvement in mood and anxiety typically takes several weeks because the brain needs time to adjust. Receptors sensitivity changes, certain genes and internal cell signals shift and connections between neurons (and even new neurons in areas like the hippocampus) strengthen. In short, SSRIs quickly raise serotonin levels, but symptom relief comes only later as the brain adapts.
Does Depression Equal Low Serotonin?
The “chemical imbalance” model—that depression is caused by low serotonin—has been a popular and influential simplification. But decades of research show depression is multi‑factorial, involving genetics, life stressors, altered neural circuits, inflammation, endocrine factors and social/environmental contributors. Studies that directly measure serotonin or its metabolites in humans have produced inconsistent results. Large reviews and modern syntheses conclude there is not definitive, consistent evidence that a simple, generalizable “serotonin deficit” underlies mood disorders such as depression for everyone.
That said, for many people, serotonin signaling clearly plays a role. Drugs that modulate serotonin can relieve symptoms for a substantial proportion of patients, which indicates serotonergic systems are important in mood and anxiety regulation even if low serotonin is not the whole story.
Why Some People Don’t Respond to SSRIs
There are several reasons SSRIs may not help everyone. First, depression and anxiety can have many causes. If someone’s symptoms are mainly the result of things other than serotonin—like inflammation, undiagnosed bipolar disorder, substance use or major life stress—SSRIs may not work well. Second, genetic differences also affect response. Variations in genes involved in making serotonin, transporting or sensing it or in drug‑metabolizing enzymes (like CYPs) can alter how a person reacts.
Sometimes SSRIs don’t help because the brain adjusts: Raising serotonin can cause receptors to change or use up the stores neurons keep, which can reduce the drug’s effect. Practical issues matter too — if the dose is too low or the medicine isn’t taken long enough, people often don’t get the chance to improve, and stopping early can look like the drug didn’t work. Other health problems or interactions with other medications can also get in the way.
Clinicians weigh these factors when deciding whether to prescribe an SSRI. They consider symptom severity, patient history, prior treatment responses, side‑effect profiles and patient preferences. For mild to moderate symptoms, psychotherapy (especially cognitive behavioral therapy or CBT), lifestyle interventions like exercise, sleep and diet and social supports are often recommended alongside or before medication. For moderate to severe depression, or when psychotherapy alone is insufficient, SSRIs are commonly offered because of their proven efficacy and relatively favorable safety compared with older antidepressants.
Common Side Effects of SSRIs
SSRIs are generally better tolerated than older classes such as monoamine oxidase inhibitors (MAOIs) and tricyclic antidepressants, but they have a characteristic side‑effect profile. Many side effects are dose‑dependent and most are transient, improving over days to a few weeks. Common adverse effects include:
- Gastrointestinal symptoms: nausea, diarrhea, indigestion—often early and transient.
- Sexual dysfunction: decreased libido, delayed orgasm or ejaculation, anorgasmia. These effects can persist as long as the drug is taken and are a major reason for discontinuation.
- Sleep disturbances: insomnia or, less commonly, excessive sleepiness. Some SSRIs can cause vivid dreams.
- Headache: mild headaches are common initially.
- Anxiety or agitation: paradoxical increase in anxiety or restlessness can occur at the start of treatment.
- Sweating: increased night sweats or generalized sweating.
- Weight changes: modest weight gain over months is commonly reported; some people lose weight initially.
- Tremor: mild fine tremor may appear.
 It is important to note that some situations need extra care. If you’re pregnant or breastfeeding, different SSRIs have different risks, so your clinician will weigh your mental‑health needs against any potential risk to the baby and make a decision that fits your situation. Taking many medicines at once is also important to consider. SSRIs are processed by liver enzymes (CYPs), so taking them along with other drugs can raise or lower SSRI levels. Always check for interactions before combining medications. SSRIs usually work best alongside psychotherapy, and if they don’t help, doctors may try switching drugs, adding another medication or using non‑drug treatments like electroconvulsive therapy (ECT) or transcranial magnetic stimulation (TMS).
It is important to note that some situations need extra care. If you’re pregnant or breastfeeding, different SSRIs have different risks, so your clinician will weigh your mental‑health needs against any potential risk to the baby and make a decision that fits your situation. Taking many medicines at once is also important to consider. SSRIs are processed by liver enzymes (CYPs), so taking them along with other drugs can raise or lower SSRI levels. Always check for interactions before combining medications. SSRIs usually work best alongside psychotherapy, and if they don’t help, doctors may try switching drugs, adding another medication or using non‑drug treatments like electroconvulsive therapy (ECT) or transcranial magnetic stimulation (TMS).
Less Common but Important Risks
Serotonin syndrome is a rare but potentially life‑threatening reaction marked by high fever, agitation, rapid heart rate, dilated pupils, muscle rigidity and autonomic instability. Risk of serotonin syndrome rises when SSRIs are combined with other serotonergic drugs. Hyponatremia (low sodium), especially in older adults, can cause confusion, falls or seizures. SSRIs modestly increase bleeding risk by affecting platelets, particularly when taken with NSAIDs or anticoagulants.
In people with undiagnosed bipolar disorder, SSRIs can trigger mania or hypomania, so screening is important. Abruptly stopping SSRIs may cause withdrawal symptoms such as dizziness, “brain zaps,” insomnia, irritability or nausea. Tapering off the dose reduces this risk. In those under 25, antidepressants carry a small increased risk of suicidal thoughts, so close monitoring early in treatment and after dose changes is essential.
Many people tolerate SSRIs well long term and benefit from them, but regular follow‑up is needed to review effectiveness, side effects (including those relating to sexual function), suicidal risk and relevant labs. When considering discontinuation of SSRIs, clinicians balance relapse risk versus side effects.
Natural Ways to Support Healthy Serotonin Levels
The following natural strategies don’t replace clinical treatment for major depression or severe anxiety, but they can complement medical care and may support mood and overall brain health.
Diet and Nutrients
Eating to support healthy serotonin levels starts with getting enough of its building block, tryptophan. Tryptophan can be found in foods like turkey, chicken, eggs, dairy, tofu, soy, nuts, seeds and oats. Including carbohydrates as part of a balanced meal can help tryptophan enter the brain by triggering insulin and shifting competing amino acids into muscle.
Certain vitamins and minerals—especially B6, folate (B9), B12, magnesium and iron—are important cofactors for serotonin production, so deficiencies can impair synthesis. Omega‑3 fatty acids like EPA and DHA also support brain health and have shown modest antidepressant effects in some studies.
Exercise
Regular aerobic exercise—about 30 minutes most days—boosts mood by increasing availability of serotonin precursors, promoting neuroplasticity and raising endorphins and BDNF (brain-derived neurotrophic factor), a protein in the brain that supports neuronal function and growth. Both moderate and vigorous activity are beneficial.
Sleep and Circadian Health
Maintaining a consistent sleep schedule and getting sunlight exposure helps regulate serotonin–melatonin pathways, while poor sleep disrupts neurotransmitter balance and worsens mood. Bright morning light or light therapy can improve mood and circadian rhythms and is an effective treatment for seasonal affective disorder.
Stress Reduction and Psychotherapy
Chronic stress lowers serotonin function. Stress‑reduction techniques such as mindfulness, cognitive behavioral therapy, meditation and other stress‑management practices reduce stress hormones and strengthen mood circuitry.
Sunlight and Light Therapy
Bright light exposure—especially in the morning—can improve mood and stabilize circadian rhythms. Controlled light therapy is also an effective treatment for seasonal affective disorder.
Gut Health
Gut health also matters. The gut microbiome interacts with serotonin systems through enteric serotonin production and gut–brain signaling, so a diverse diet rich in fiber, fermented foods and pre/probiotics may support microbiome health. Evidence is still emerging but promising.
 Healthy Social Connection and Activities
Healthy Social Connection and Activities
Healthy social connections, purposeful activities and behavioral activation provide positive reinforcement and can improve mood independently of medication. Finally, avoid substances that impair serotonin function—excessive alcohol, recreational drugs and nicotine worsen mood over time and can interfere with treatment.
Selective Serotonin Reuptake Inhibitor Drugs Aren’t a Universal Fix
Bottom line: SSRIs increase extracellular serotonin and can meaningfully reduce symptoms of depression and anxiety for many people, but they’re not a one‑size‑fits‑all “fix” for a supposed universal serotonin deficiency. Because depression and anxiety have many causes, SSRIs are effective for many but not all patients. If you’re considering an SSRI, discuss personalized risks and alternatives with a clinician who can match treatment to your history and symptoms.




