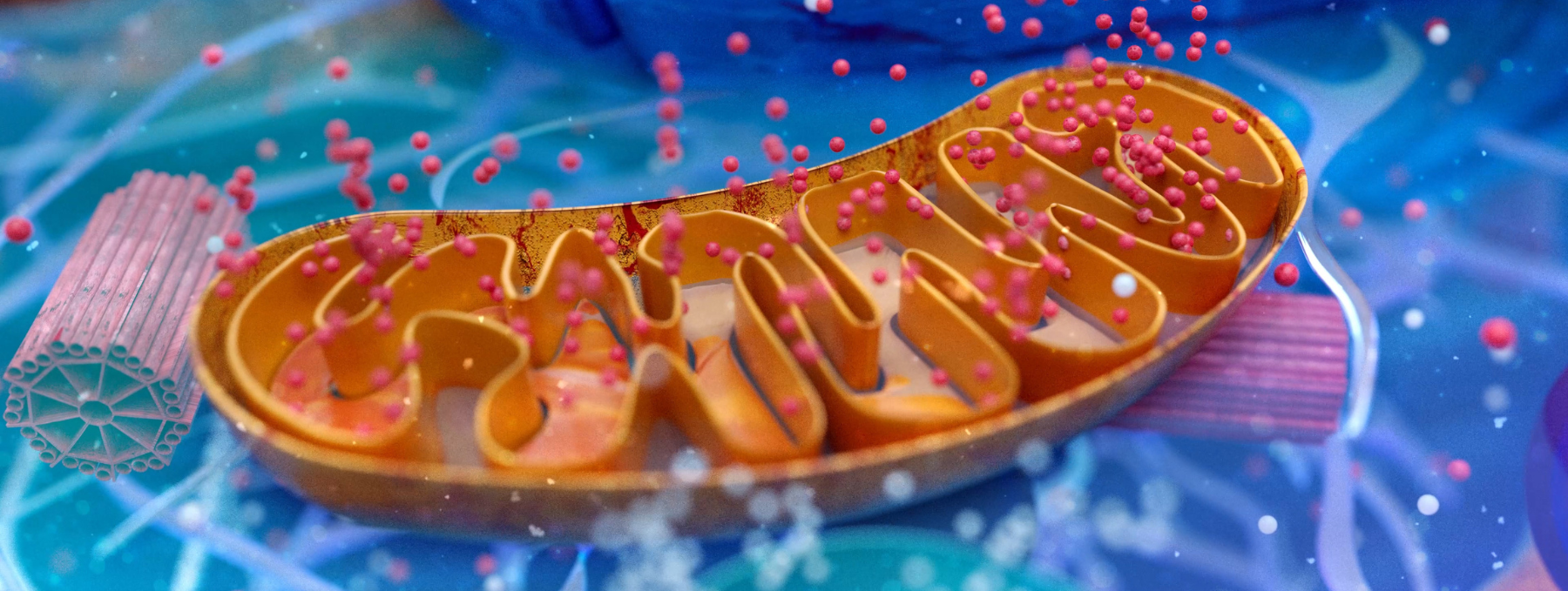
When we talk about mood, terms like “brain chemistry” and “serotonin” often come up. But beneath those headlines lies a quieter, essential story: the role of cellular energy. Mitochondria — tiny structures inside nearly every cell that produce the energy molecule ATP — play a surprising part in how your brain makes and uses serotonin, and that connection helps shape mood, motivation and mental clarity.
What Mitochondria Do: A Quick Primer
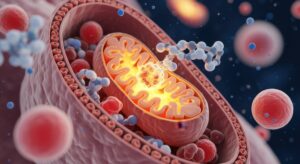 Mitochondria are the cell’s power plants, as they convert nutrients into ATP—the chemical fuel that powers processes like neuron firing, protein recycling and neurotransmitter production. Located throughout cells but especially abundant in energy-hungry tissues like the brain and muscles, mitochondria also help regulate cellular calcium levels, which is vital for signaling and neurotransmission.
Mitochondria are the cell’s power plants, as they convert nutrients into ATP—the chemical fuel that powers processes like neuron firing, protein recycling and neurotransmitter production. Located throughout cells but especially abundant in energy-hungry tissues like the brain and muscles, mitochondria also help regulate cellular calcium levels, which is vital for signaling and neurotransmission.
Mitochondria send out biochemical signals that influence cell growth, cell survival and the cleanup of damaged cellular components. They also produce reactive oxygen species (ROS)—molecules that at low levels act as normal signaling agents but that can cause oxidative damage and impair cell function when produced in excess. Together, these roles make mitochondria central not only to energy supply but also to overall cellular health and communication.
Why Serotonin Needs Energy
Serotonin is synthesized from the amino acid tryptophan through a series of enzymatic reactions that require ATP to run efficiently, so when cellular energy is low these biochemical steps slow down and serotonin production can drop. After neurons make serotonin, they use energy to pack it into tiny storage sacs (vesicles), move those sacs along internal “tracks” to the release sites and push the serotonin out into the gap between cells—steps that all require ATP. Once released, serotonin is taken back up by transport proteins that also need energy to remove and recycle it, and the enzymes that break down serotonin depend on the cell’s metabolic state as well.
Altogether, the synthesis, storage, release, clearance and metabolism of serotonin require a lot of energy. Therefore, if serotonin-making neurons don’t have enough energy, several things can go wrong at once: The brain makes less serotonin, stores and releases it less effectively and clears or breaks it down differently. That lowers how much serotonin is available and changes when and how strongly neurons communicate, which can then affect mood, thinking and behavior.
Mitochondria Affect Serotonin Both Directly and Indirectly
Mitochondria affect serotonin in two ways. Directly, they provide the ATP needed for the enzymes that make serotonin, the transporters that pack it into storage sacs and the proteins that clear it from the synapse. So if mitochondria fail and energy falls, those steps are weakened. Indirectly, mitochondria control the cell’s balance of reactive molecules and calcium levels, both of which influence enzyme activity and how receptors respond. When oxidative stress or calcium is out of whack, serotonin metabolism and receptor function can be disrupted. The link goes both ways: Serotonin activity turns on receptors and internal signals that can change how mitochondria grow, move and work.
In short, mitochondria affect serotonin, and serotonin can in turn affect mitochondrial behavior. These feedback loops let cells match energy production to demand — for example, when neurons are highly active, serotonin-related signals can tell mitochondria to make more ATP. However, if that coordination breaks down, it can lead to lasting energy shortfalls and poor neurotransmission, which are seen in some mood disorders.
Evidence Links Mitochondrial Problems to Mood Disorders
 Clinical and laboratory studies have repeatedly identified mitochondrial abnormalities in people with depression, bipolar disorder and chronic fatigue, including reduced mitochondrial respiration, altered mitochondrial DNA and markers of oxidative damage in brain tissue or blood cells. In experimental models, deliberately impairing mitochondrial function can produce behaviors resembling depression or fatigue in animals, while interventions that improve mitochondrial performance sometimes alleviate those behaviors.
Clinical and laboratory studies have repeatedly identified mitochondrial abnormalities in people with depression, bipolar disorder and chronic fatigue, including reduced mitochondrial respiration, altered mitochondrial DNA and markers of oxidative damage in brain tissue or blood cells. In experimental models, deliberately impairing mitochondrial function can produce behaviors resembling depression or fatigue in animals, while interventions that improve mitochondrial performance sometimes alleviate those behaviors.
These findings do not imply that mitochondria are the sole cause of mood disorders—genetics, life stress, inflammation, sleep and social environment also play major roles. However, mitochondrial dysfunction is a consistently implicated biological factor that helps explain how cellular energy deficits can contribute to psychiatric symptoms.
How Energy Shortfalls Can Translate Into Feelings
Low ATP in brain cells makes neurons less responsive and reduces effective neurotransmission, which can produce core symptoms of mood disorders such as low motivation, cognitive fog, slowed thinking and persistent tiredness. Because many neurotransmitter processes require energy, even modest deficits can change the timing and strength of neural signaling, negatively affecting concentration, decision-making and the ability to sustain goal-directed activity. When cellular energy shortages specifically dampen serotonin signaling, people may experience increased anxiety, reduced resilience to stress, disrupted sleep and a diminished capacity to feel pleasure from activities that once brought enjoyment.
These functional changes in neural circuits can also make it harder for the body to regulate stress, making everyday challenges feel harder to cope with. Meanwhile, inflammation or chronic psychological stress can damage mitochondria and create a vicious feedback loop—stress leads to mitochondrial impairment, which worsens neurotransmission and increases sensitivity to further stress. As a result, what begins as temporary fatigue or low mood can become chronic without interventions that restore cellular energy and break the cycle.
Lifestyle Factors That Support Mitochondria and Serotonin
Supporting your mitochondria is a practical way to protect serotonin signaling and overall brain health. Small, consistent lifestyle changes can boost cellular energy, improve neurotransmission and reduce risk factors that erode mood over time. Following are some lifestyle factors that can help support mitochondrial health and optimum serotonin levels.
- Regular physical activity: Exercise stimulates the creation of new mitochondria and improves mitochondrial efficiency. It also boosts serotonin release and enhances mood.
- Balanced diet: Nutrients like omega-fatty acids, B vitamins (especially B6, B9/folate, and B12), coenzyme Q10, magnesium and adequate protein (for tryptophan) support mitochondrial enzymes and neurotransmitter synthesis.
- Sleep and circadian rhythm: Mitochondrial processes follow circadian patterns. Poor sleep disrupts mitochondrial function and neurotransmitter balance; good sleep supports both.
- Stress management: Chronic stress drives inflammation and oxidative damage that harm mitochondria. Mindfulness, therapy, social support and paced breathing can reduce that burden.
- Avoiding toxins and excessive alcohol: These increase oxidative stress and can impair mitochondrial respiration.
Serotonin and Mitochondria: Clinical and Therapeutic Implications
 Emerging research suggests that targeting mitochondrial function could help with mood symptoms. Exercise programs, dietary strategies and mitochondria-targeted compounds — including certain antioxidants — have shown promise in studies. Traditional antidepressants also interact with cellular energy pathways in complex ways, and some treatments may indirectly improve mitochondrial function as part of their therapeutic effects. Because mood disorders are biologically diverse, mitochondrial-focused approaches are unlikely to help everyone equally; personalized strategies may be more effective, but routine clinical tests of mitochondrial health are not yet standard practice and research is ongoing.
Emerging research suggests that targeting mitochondrial function could help with mood symptoms. Exercise programs, dietary strategies and mitochondria-targeted compounds — including certain antioxidants — have shown promise in studies. Traditional antidepressants also interact with cellular energy pathways in complex ways, and some treatments may indirectly improve mitochondrial function as part of their therapeutic effects. Because mood disorders are biologically diverse, mitochondrial-focused approaches are unlikely to help everyone equally; personalized strategies may be more effective, but routine clinical tests of mitochondrial health are not yet standard practice and research is ongoing.
It is important to note that mitochondrial findings in mood disorders may reflect cause, consequence or both—in short, correlation does not prove causation. Mitochondrial dysfunction is only one contributor among psychological, social and other biological factors. Supplements or “mitochondria-boosting” treatments are not substitutes for evidence-based care for clinical depression or other psychiatric conditions, so it is important to discuss any new interventions with a clinician.
Boost Mood By Supporting Your Cellular Powerhouses
Mitochondria and serotonin are connected through multiple biochemical pathways, and cellular energy production influences how effectively serotonin is made, stored, released and recycled. While mitochondrial dysfunction is not the sole cause of mood disorders, it is a meaningful biological contributor, so supporting the mitochondria — your cellular “powerhouses” — is one practical route to better brain function and potentially better mood. Supporting energy metabolism complements other mental-health strategies; think holistically and remember that small habits add up. Regular movement, consistent sleep, whole foods with adequate micronutrients and stress management are practical steps that support mitochondria, neurotransmitter balance and mood.